Effect of Patchouli Alcohol, a Tricyclic Sesquiterpene, on SPEM Malignant Progression
Authors
Yifei Xu1,*, Liyao Tang3, Weijian Zhang1, Xinxin Hong1, Jianqu Xu1, Gautam Sethi2, Shaoju Guo1,*
Affiliations
- Institute of Gastroenterology, Shenzhen Traditional Chinese Medicine Hospital, The Fourth Clinical Medical College of Guangzhou University of Chinese Medicine, Shenzhen 518033, China
- Department of Pharmacology, Yong Loo Lin School of Medicine, National University of Singapore, Singapore 117600, Singapore
- School of Pharmaceutical Sciences, Jishou University, Jishou 416000, China
Corresponding Author
Yifei Xu (xyf2995@gzucm.edu.cn)
Shaoju Guo (gsj1080@163.com)
Introduction
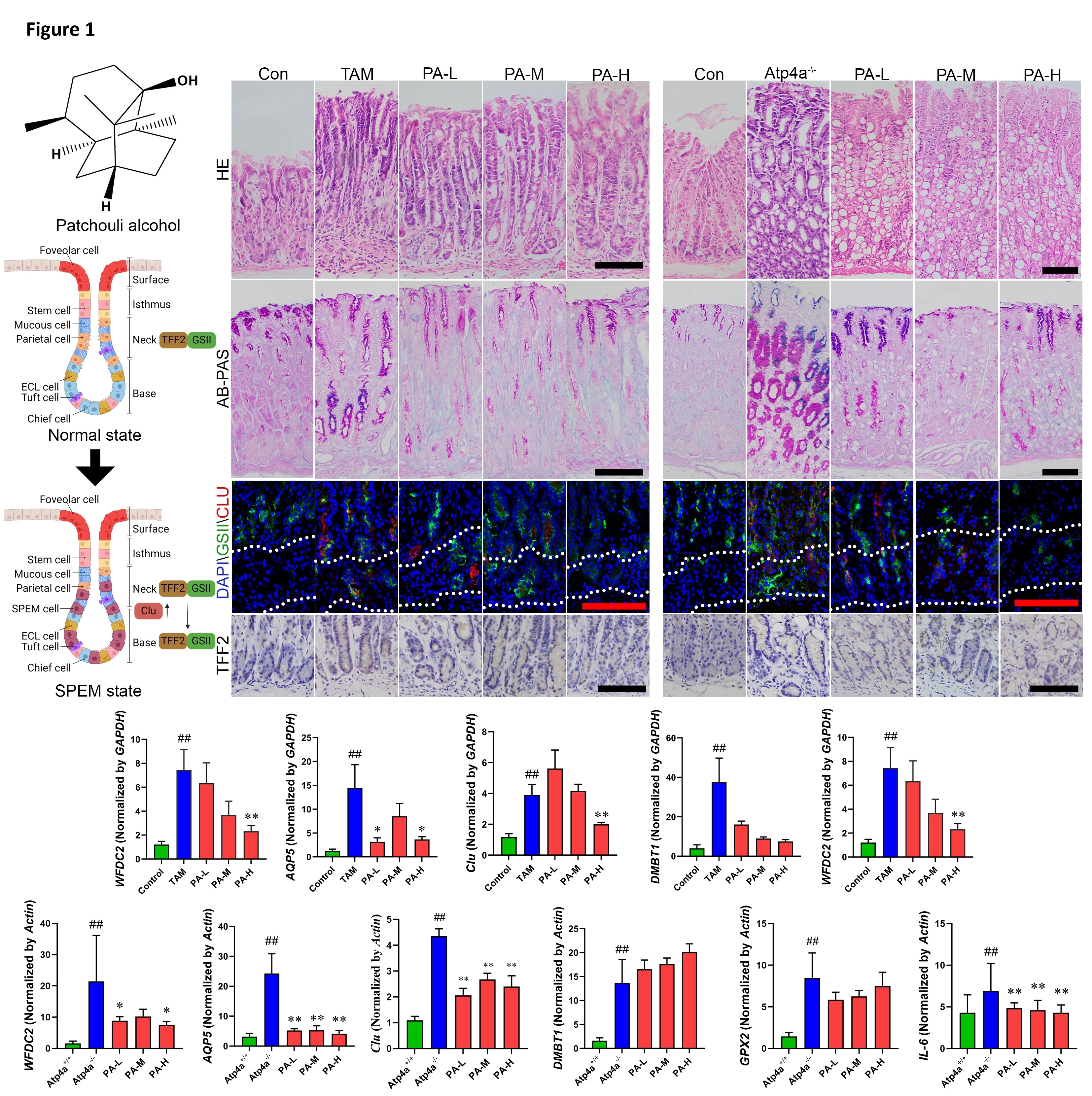
The origin of spasmolytic polypeptide-expressing metaplasia (SPEM), whether it arises from chief cell trans-differentiation or abnormal differentiation of stem cells, remains controversial. The occurrence of SPEM is associated with alterations in homeostasis and epigenetic regulation within gastric mucosal cells, leading to heightened susceptibility to malignant progression under persistent chronic inflammation. Pogostemon cablin (Blanco) Benth., a traditional Chinese medicine, is widely used in the treatment of gastrointestinal diseases. The primary active component, patchouli alcohol (PA), has demonstrated potent anti-Helicobacter pylori (H. pylori) and anti-inflammatory activities. In this study, the effects of PA on the malignant progression of SPEM were investigated.
Methods
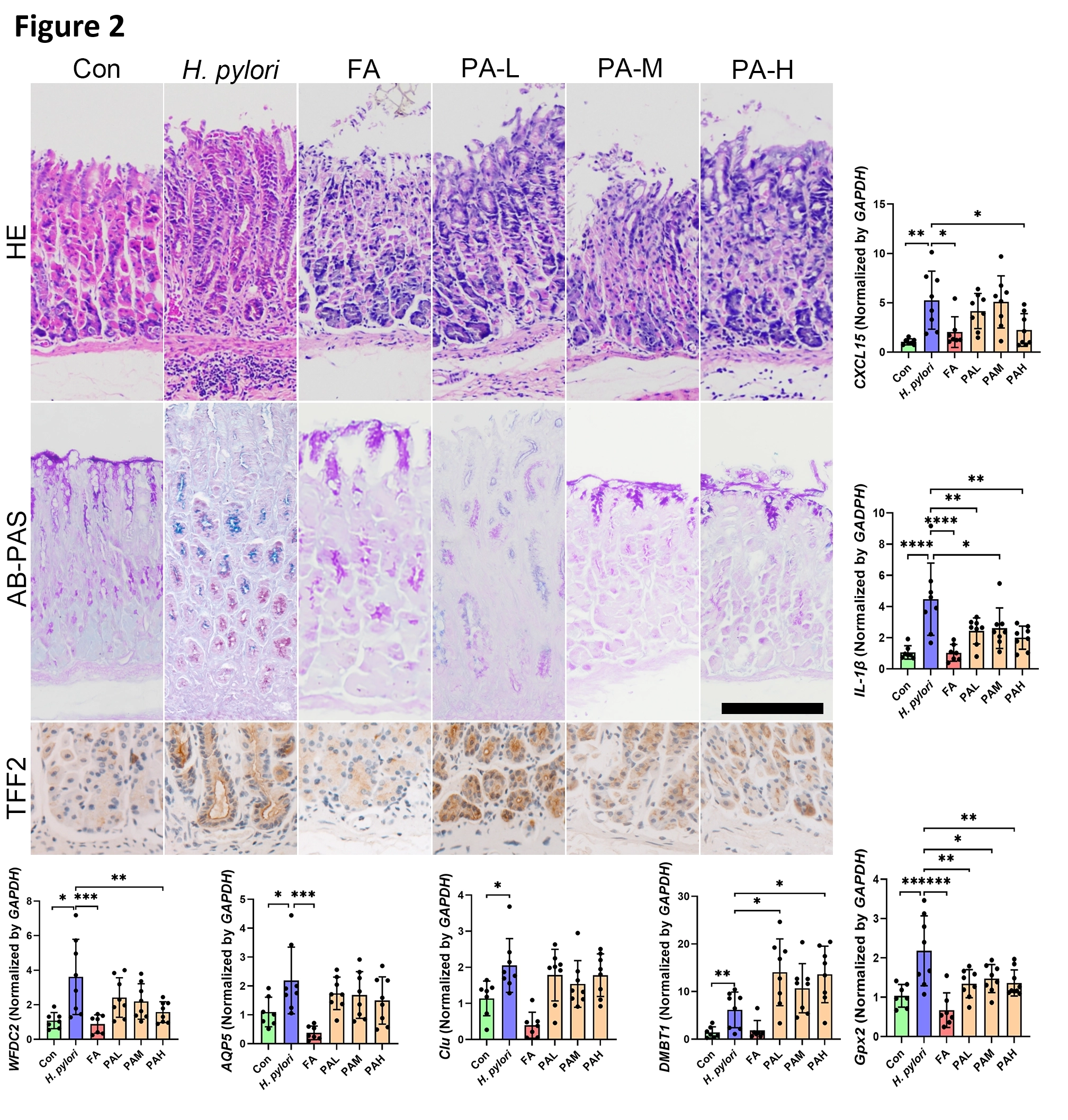
SPEM mice induced by high dose tamoxifen, atp4a knockout and H. pylori were treated with PA at 15, 30 and 60 mg/kg. The pathology, mucus secretion, SPEM status, and malignant progression were assessed using HE staining, AB-PAS staining, immunohistochemistry, immunofluorescence, and Q-PCR.
Results
PA did not show significant improvement in the pathological condition of gastric mucosa or the occurrence of acute SPEM (TFF2 and GSII), but it did enhance gastric mucus secretion in three models and H. pylori-induced chronic SPEM. Meanwhile, PA downregulated the expression of WFDC2 in all three SPEM models, as well as the expression of AQP5 and Clu in tamoxifen and Atp4a knockout SPEM model. Besides, the expressions of REDOX gene GPX2 and inflammatory factor IL-6 were reduced in tamoxifen and Atp4a knockout SPEM model, respectively. In H. pylori-induced SPEM mice, PA decreased the expressions of inflammatory factors cxcl15 and IL-1β, as well as downregulated the REDOX gene GPX2. Additionally, it upregulated the tumor suppressor factor DMBT1.
Conclusion
PA didn’t exert a significant impact on the occurrence of acute SPEM; however, it significantly inhibits chronic SPEM and its malignant progression through suppression on inflammation and oxidative stress, and consequently contributes to maintain gastric mucosal homeostasis.