Effect of Helicobacter pylori Infection on Survival Outcomes of Patients Undergoing Radical Gastrectomy after Neoadjuvant Chemotherapy: A Multicenter Study in China
Authors
Qi-Chen He ,Wen-Wu Qiu ,Ji-Xun He
Introduction
Neoadjuvant chemotherapy (NAC) has been confirmed to improve the prognosis of patients with advanced gastric cancer (AGC). However, no study has investigated whether Helicobacter pylori (HP) infection affects the postoperative survival of patients who receive NAC.
Methods
This multicenter retrospective cohort study included 307 patients with AGC who underwent laparoscopic radical gastrectomy after NAC at three hospitals in China between January 1, 2016, and April 31, 2020. The HP infection status was determined by histopathology. Cox regression was used to assess prognostic factors for survival. Kaplan-Meier was used for survival analysis.
Results
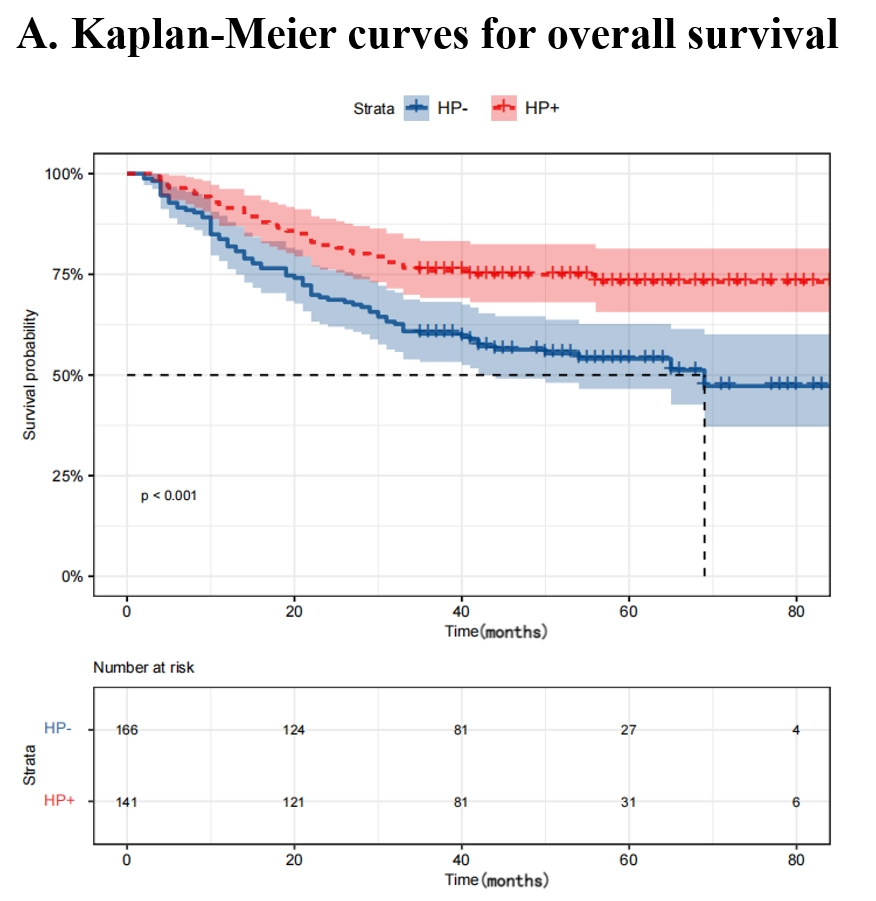
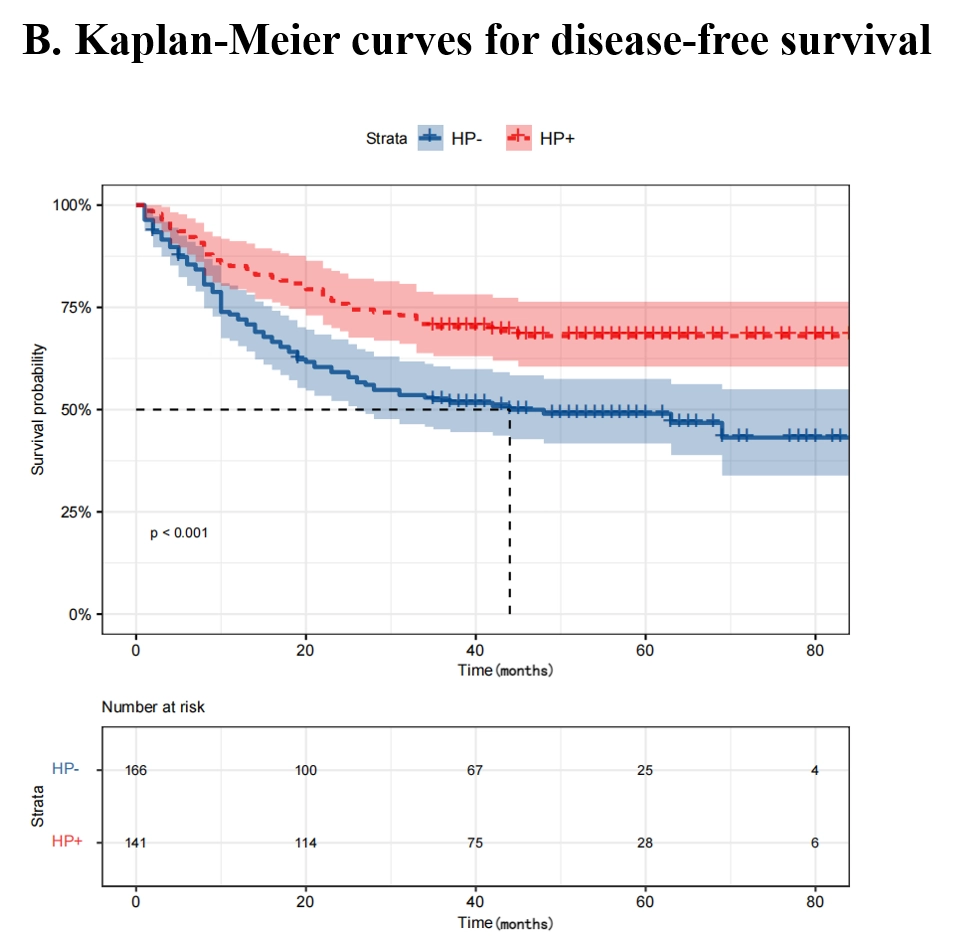
The HP+ group and the HP- group included 141 (46%) and 166 (54%) cases respectively. The 3-year overall survival (OS) and disease-free survival (DFS) of the HP+ group were significantly better than the HP- group (3-year OS: 75.9% vs. 60.2%, 3-year DFS: 70.2% vs. 52.3%; All P<0.001). For the HP+ group, ypTNM Stage III (HR, 4.00; 95% CI, 1.11–14.39; P=0.034), NAC ≥4 cycles (HR, 0.43; 95% CI, 0.20–0.90; P=0.026), and adjuvant chemotherapy (AC) ≥4 cycles (HR, 0.20; 95% CI, 0.09–0.48; P<0.001) are independent prognostic factors for OS. In the cohort of HP+ patients who received ≥4 cycles of NAC, the prognosis of patients who received ≥4 cycles of AC after surgery was better than that of patients who received <4 cycles of AC (3-year OS: 92.5% vs 71.4%; P=0.042).
Conclusion
Following NAC, HP+ patients with AGC exhibit better prognosis than that of HP- counterparts. For potentially resectable HP+ AGC patients, radical surgery following ≥4 cycles of NAC with ≥4 cycles of sequential AC might be recommended to improve survival.
Keywords
Neoadjuvant chemotherapy; Helicobacter pylori; Gastric cancer; Gastrectomy
Kaplan-Meier curves of overall survival and disease-free survival for H. pylori positive vs H. pylori negative after surgery